Abstract
Introduction: Interstitial lung changes persist in some patients after COVID-19 hospitalisation.
Aim: To characterise longitudinal pulmonary changes due to COVID-19 using 129Xe and 1H MRI.
Methods: Patients with abnormal CT or 1H MRI underwent MRI and PFTs up to 106 weeks after hospitalisation. MRI protocol: 129Xe gas transfer (key metric: red blood cell to membrane fraction, RBC:M), 129Xe ventilation, lung perfusion and structural imaging. Longitudinal comparisons (24 vs 52 weeks) and correlations were assessed using Wilcoxon Signed Rank and Spearman's rank.
Results: 23 patients (median age: 68(range: 53-78) years, 87% male) underwent MRI at 23(6-33)(n=13), 54(42-71)(n=18) and 106(98-117)(n=7) weeks after hospital admission.
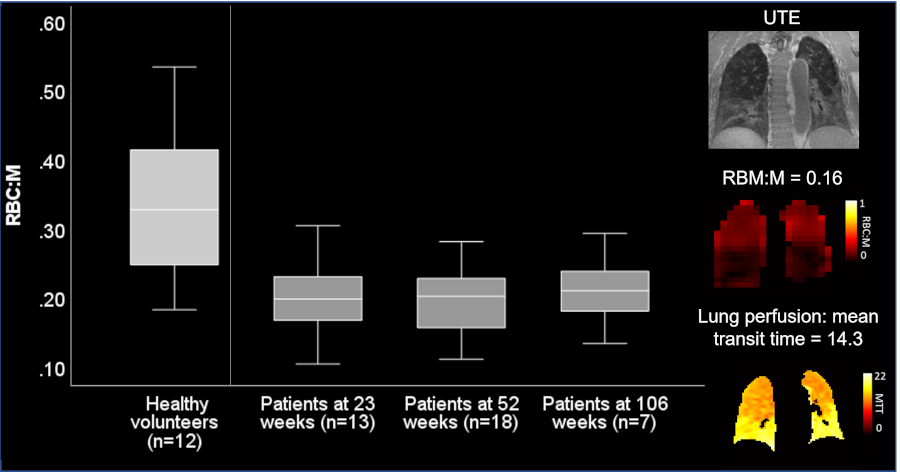
Patients had decreased RBC:M compared to older controls and low transfer factor Z-score at 24, 52 and 106 weeks (median TLCOz<-2.2 at all visits).
Ventilation defect percentage was <6% for all patients.
There was no longitudinal change (n=8) in 129Xe gas transfer or TLCOz between 24 and 52 weeks. There was a significant decrease in FEV1/FVC Z-score and an increase in FVC Z-score (p=0.018; p=0.043). At 24 and 52 weeks, RBC:M correlated with TLCOz (r=0.661, p=0.038; r=0.709, p=0.015).
Conclusion: Xenon gas transfer remains impaired two years post hospitalisation in this cohort.
Fig 1: RBC:M alongside healthy control data (57(41-68)years, 67% male).