Abstract
Aim
This study aims to investigate the spectrum and extent of structural lung changes (SLC) on chest CT scans (cCTs) of patients in the European Bronchiectasis registry (EMBARC).
Methods
cCTs from EMBARC patients were analyzed semi-automatically using the validated Bronchiectasis Scoring Technique for CT (BEST-CT). BEST-CT scores are expressed as % of total lung volume. Scoring items are: consolidation/atelectasis (%ATCON), bronchiectasis with and without mucus plugging (%BEMP, %BEwMP), airway wall thickening (%AWT), mucus plugging (%MP), ground-glass opacities (%GGO), emphysema/bullae(%EMPBUL), healthy airways and parenchyma (%HA,%HP). Also, composite scores were calculated: Total BE (%TBE = %BEMP + %BEwMP), total airway disease (%AD = %TBE + %MP + %AWT), total MP (%TMP = %BEMP + %MP), total inflammatory changes (%TinF = %ATCON + %BEMP +%MP) and total disease (%DIS = all but %HA & %HP).
Results
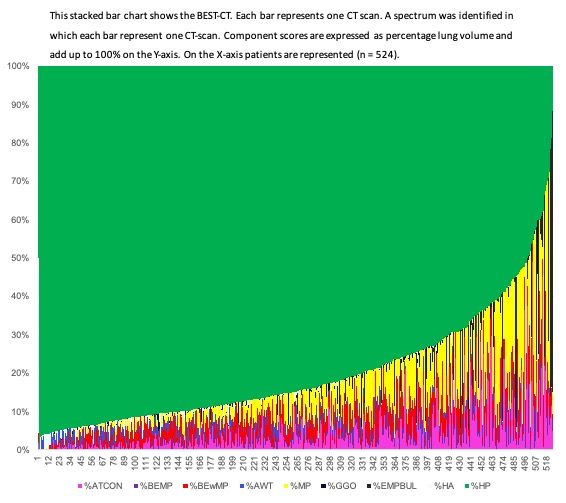
524 patients were analyzed, age 66 (55 ? 74) years, female 63%, FEV1%pred 79 (62-91). We observed heterogeneity between patients, see figure 1. Average values across the population were %TBE 4.6 (2.3 ? 7.7), %AD 9.9 (5.9 ? 17.5), %TMP 4.2 (1.2 ? 8.1), %TinF 8.3 (3.5 ? 16.7) and %DIS 14.9 (9.1 ? 25.9).
Discussion
Considerable heterogeneity in spectrum and extent of SLC was observed in a large group of EMBARC patients. We show the potential of BEST-CT to phenotype SLC in BE patients and to incorporate scoring into multicentre registries.